When Dr. De’Broski R. Herbert was a child in southern Mississippi, his great grandmother would warn him against going outside barefoot. “That was such a frustrating and confusing thing to hear as a 5-7 year old child,” recalled Dr. Herbert. “It didn’t make much sense to me at the time.” However, years later, while taking a course on parasites in college, Dr. Herbert understood the scientific basis for his great grandmother’s warning: parasites in the soil.
Dr. Herbert is now an immunologist who studies parasitic organisms to understand how they change human biology, with the goal of developing improved therapeutic options for a variety of diseases. In his recent research, he has turned to the parasitic worm, Schistosoma mansoni, which can enter the skin undetected. The findings of this research reveal novel mechanisms used by S. mansoni parasitic worms to prevent a pain response. Dr. Herbert hopes these results point the way towards novel medications for pain management as well as therapies to treat S. mansoni infection.
New Perspectives on Parasites
Dr. Herbert first became interested in parasites1Parasite: An organism that lives in or on a host organism and survives at the expense of the host. https://www.cdc.gov/parasites/about/index.html during college, and he has devoted his career to understanding and learning from these creatures. “Parasites are some of the most fascinating, intricate, and complicated organisms on Earth,” commented Dr. Herbert.
A parasite is any organism that lives in or on another organism, called the host organism2Host organism: An organism that is infected with or fed on by a parasitic organism. https://www.biologyonline.com/dictionary/host. Some parasites live on the surface of their hosts, like fleas3Fleas: Small insects that survive on the blood of human or animal hosts. https://www.cdc.gov/fleas/about/index.html, ticks4Ticks: Small insects that survive on the blood of human or animal hosts and are known to transmit serious diseases including Lyme disease. https://www.cdc.gov/ticks/about/index.html, and lice5Lice: Small insects that survive on the blood of human or animal hosts. https://www.cdc.gov/lice/about/index.html. These are known as ecto-parasites6Ecto-parasite: A parasite that lives outside of another animal but does not kill it, including fleas, ticks, and lice. https://www.amentsoc.org/insects/glossary/terms/ectoparasite/. Other parasites, called endo-parasites7Endo-parasite: A parasite that lives inside the body of another animal but does not kill it, including types of parasitic worms. https://www.collinsdictionary.com/us/dictionary/english/endoparasite, enter the host’s body and live inside it, including many types of parasitic worms.

Common parasites that infect humans include fleas, ticks, lice, and different types of parasitic worms.
[Source: https://microbeonline.com/parasitic-infections-source-of-infection-mode-of-transmission-and-prevention/]
Hookworms8Hookworm: A type of parasitic worm found in contaminated soil; named for the hook-like shape of its head. https://www.cdc.gov/sth/about/hookworm.html, a type of parasitic worm in the soil where Dr. Herbert grew up, can enter the host directly through the skin, for example through a child’s bare foot, and cause infection. As Dr. Herbert’s great grandmother knew well, wearing shoes protects a child’s feet from invasion by hookworms and other parasites in the soil.
Parasites are different from other organisms like viruses and bacteria that cause human disease. This makes parasites especially interesting for scientists. Unlike many viruses and bacteria that infect humans, parasites depend on the continued survival of their host for their own survival. This means they adapt to living inside their host and have developed a variety of mechanisms to remain relatively undetected. Dr. Herbert believes the key to many new medications lies in understanding how parasites manipulate the human body. He hopes to apply this knowledge to treat human diseases.
Parasitic worms are of particular interest to Dr. Herbert because they are so large compared to other disease-causing organisms. The adult worms of some species can be seen by the naked eye without any magnification. While some parasitic worms do cause skin irritation upon infection and can lead to digestive symptoms and other health issues, other parasitic worms, like Schistosoma mansoni, can remain inside the human body for years or decades without causing any symptoms at all.
Scientists have been studying parasitic worms for decades because of their ability to evade or manipulate the immune system9Immune system: Network of organs, tissues, and cells in the body that fight infection and prevent disease. https://immunologyexplained.aai.org/what-is-immunology/what-is-the-immune-system/. “These are organisms that have evolved with humans to live within our bodies for years or decades,” explained Dr. Herbert. “They have many different strategies to prevent an immune response and most of these strategies are still unknown. This is a great opportunity for basic scientific discovery in the laboratory.” Indeed, researchers have shown that parasitic worms regulate the immune system in ways that can also benefit the host. The worms do provoke an immune response, but that response is very quiet and doesn’t lead to much tissue damage. It also doesn’t kill the worms.
Dr. Herbert continued this line of research by thinking like a worm: “If I was a worm, and I had evolved a way to evade one biological system inside the host, why would I stop there?” Dr. Herbert asked. He hypothesized that the effects of parasitic worms on their hosts would go beyond just the immune system. For the worms to enter the body undetected and remain undetected, they had to influence the nervous system10Nervous system: A system of the body including the brain, spinal cord, and nerves, that together help you think, move, and feel. https://my.clevelandclinic.org/health/body/21202-nervous-system as well.
The Life Cycle of Schistosoma mansoni
Schistosoma mansoni is part of the Schistosoma family of parasitic worms, a type of flatworm11Flatworm: A type of worm, often parasitic, characterized by its soft body and flat shape. https://www.britannica.com/animal/flatworm commonly known as flukes. Schistosoma species are the only flukes that cause infection by directly penetrating the skin. Around the globe, an estimated 250 million people are currently infected with Schistosoma worms. There are several types of Schistosoma worms found in different regions around the world including Latin America, the Caribbean, and some areas along the Southern coast of the US.
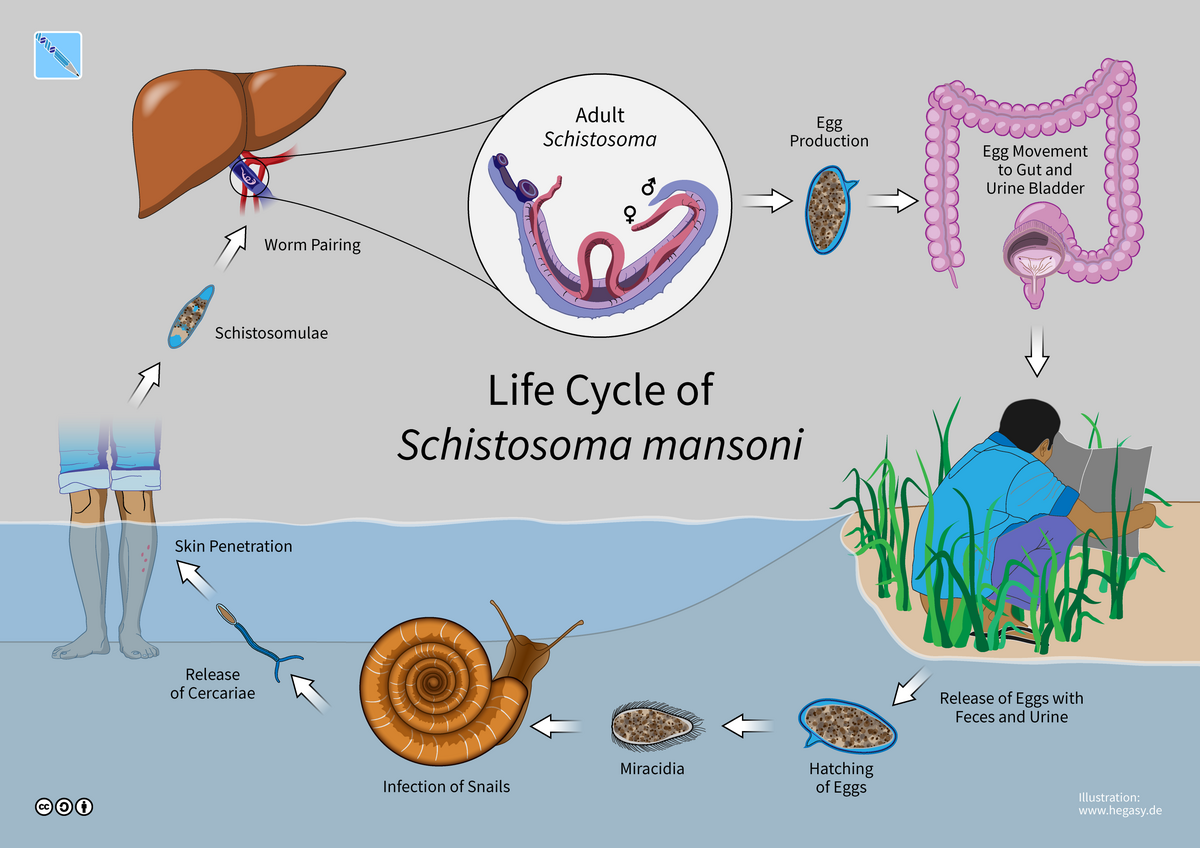
[Source: https://commons.wikimedia.org/wiki/File:03_Hegasy_Schistosomiasis_Wiki_EN_CCBYSA.png]
The life cycle of S. mansoni begins when eggs from an infected human are shed through the human’s feces and urine. The eggs hatch into larvae called miracidia, which initially infect snails. The larvae grow inside the snails and are released into the water as free-swimming cercariae, an infectious larval stage. These cercariae can directly penetrate human skin without causing any reaction including pain or itching. Once inside the body, the cercariae circulate in the blood stream and migrate to the liver, where they mature into adult worms and mate. Pairs of male and female worms move to the intestines, where they lay eggs that are shed in human urine and feces, and the cycle begins again.
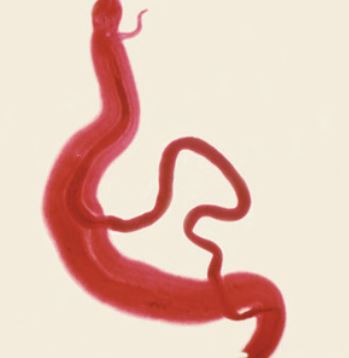
A male and female pair of adult S. mansoni parasitic worms.
[Source: https://www.cdc.gov/dpdx/schistosomiasis/index.html]
Most people infected with S. mansoni do not have any symptoms. Occasionally, people infected with S. mansoni may develop a rash where the cercariae penetrated the skin. S. mansoni can cause a serious reaction in some people known as acute schistosomiasis12Acute schistosomiasis: Acute reaction to Schistosoma eggs circulating in the body; symptoms can vary depending on the area of the body affected. https://www.who.int/news-room/fact-sheets/detail/schistosomiasis or Katayama fever. Symptoms typically begin 2-4 weeks after exposure and may include fever, cough, headaches, and abdominal pain or tenderness. These symptoms are associated with the circulation of eggs rather than the worms themselves. Schistosomiasis can also become chronic, eventually leading to problems in the intestines, liver, lungs, bladder, and genitals, depending on the site of infection.
Schistosomiasis, either with or without symptoms, can be diagnosed using laboratory tests that look for markers in the blood or S. mansoni eggs in the stool. It can be treated with medications that target parasitic worms, although multiple courses of treatment may be needed. Schistosomiasis can be prevented by avoiding contact with contaminated water.
Parasitic Worms May Suppress Pain Signals
In his research on S. mansoni, Dr. Herbert focused on specialized neurons in the skin called nociceptors13Nociceptor: Specialized neurons in the skin involved in the sensation of pain. https://www.ncbi.nlm.nih.gov/books/NBK10965/ that detect harmful or dangerous substances and sense pain. Many nociceptors express an ion channel protein called transient receptor potential vanilloid 1 (TRPV1). TRPV1 can be activated by a variety of substances or conditions, including chili pepper, acid, and heat. The activation of TRPV1 is typically associated with the sensation of pain. Dr. Herbert hypothesized that S. mansoni must have a mechanism to decrease TRPV1 activation that allows it to enter the skin without causing any pain or itching.
To test this hypothesis, Dr. Herbert isolated mouse neurons from the dorsal root ganglia14Dorsal root ganglia: Specialized neurons that line the spinal cord and transmit sensory information including pain and itch. https://www.ncbi.nlm.nih.gov/books/NBK532291/. These are specialized neurons that line the spinal cord and transmit sensory information including pain and itch.
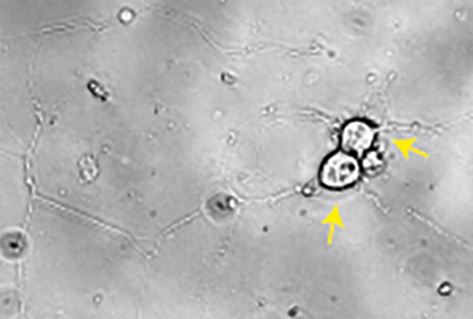
Neurons of the dorsal root ganglia.
[Source: Dr. Herbert]
Dr. Herbert already knew that these neurons would be activated when exposed to capsaicin, the active ingredient in chili peppers. As proof of the experimental design, Dr. Herbert exposed dorsal root ganglia neurons from mice to capsaicin, and the neurons became activated as expected.
Next, Dr. Herbert performed the same experiment, but this time he first exposed the dorsal root ganglia neurons to extract from S. mansoni cercariae, the infectious larvae that directly penetrate the skin to cause infection. After exposure to S. mansoni extract, the dorsal root ganglia were exposed to capsaicin. Unlike in the previous experiment, the neurons that were exposed to S. mansoni cercariae before capsaicin showed a decreased response to capsaicin. “Clearly something in the S. mansoni extract suppressed the activation of these dorsal root ganglia neurons,” explained Dr. Herbert.
Having shown that S. mansoni has an impact at the cellular level, Dr. Herbert moved into experiments in mouse models. This is a critical step for research that hopes to develop novel treatments for humans. “There are so many cool findings in cells that never translate into clinical interventions that can help humans,” added Dr. Herbert. “It’s important to conduct animal studies so we know what is going on inside a living mammal.”
To test how exposure to S. mansoni might impact animal behavior, Dr. Herbert and colleagues performed several experiments to evaluate differences in pain sensitivity in mouse models. These experiments used a previously established method that measures how long it takes a mouse to withdraw its paw when exposed to heat.
Under normal circumstances, a mouse will immediately remove any paw exposed to heat. However, Dr. Herbert found that mice who were first exposed to S. mansoni extract waited longer than control mice before removing their paw from the heat. “This is a clear demonstration of how S. mansoni interferes with a mouse’s ability to feel pain,” explained Dr. Herbert. “We wouldn’t have known this without our work in animal models.”
These findings make sense from an evolutionary perspective. The parasitic worms need their human hosts to survive to reproduce. If the human hosts felt pain or itchiness when the pathogen contacted the skin, they might scratch or swat or engage in other behaviors that prevent the parasite from entering the skin. On the other hand, if the parasite can produce molecules that prevent their hosts from feeling pain or itchiness, it makes them more likely to survive.
Dr. Herbert conducted additional experiments to determine whether the reduction in pain response that resulted from S. mansoni exposure was local, only affecting a specific area, or systemic, affecting the entire body. The results showed that the effects of S. mansoni exposure were highly localized. “We think these worms are producing novel molecules to control pain. We have never seen this before,” commented Dr. Herbert.
Future Work
Further work is needed to better understand the molecules released by S. mansoni. The experiments thus far have used a mixture of the entire worm larvae, which could include hundreds of different compounds. Dr. Herbert wants to understand which of these compounds are responsible for binding to and interacting with TRPV1, and how exactly they do so. He suspects there may be multiple compounds that affect TRPV1 in different ways. These compounds may also have impacts on nociceptors beyond TRPV1. “We’re really just at the tip of the iceberg,” added Dr. Herbert. “There’s a whole new field that we can now explore.”
In addition, Dr. Herbert hopes this work will lead to improved treatment options for people infected with parasites and a greater appreciation of the toll that parasitic infections take on the body. Parasitic infections disproportionately affect people who are poor or who live in underserved areas. These infections are often the result of suboptimal living conditions and could be prevented with improved access to health care. “We like to think of parasites as a problem somewhere else, outside the US, but parasites like hookworms are an American problem,” emphasized Dr. Herbert.
Dr. Herbert is particularly excited about the possibility that this work might lead to novel treatments for pain. Millions of people in the US and around the world suffer from pain conditions, and most of the available treatments can become addictive. The molecules used by S. mansoni to turn off pain signals in the skin are localized, making them a potential alternative to currently available systemic medications.
Dr. De’Broski R. Herbert is Professor of Microbiology and Immunology at Tulane University School of Medicine in New Orleans, Louisiana. His research focuses on understanding the mechanisms that parasitic organisms use to alter human immune and nervous systems, with the goal of developing new insights into human disease and novel treatment options. When not in the laboratory, Dr. Herbert enjoys doing yoga and spending time with his dog. “I get a lot of research ideas when I’m on the yoga mat,” added Dr. Herbert.
- Inclan-Rico JM, Stephenson A, Napuri CM, Rossi HL, Hung LY, Pastore CF, Luo W, Herbert DR. TRPV1+ neurons promote cutaneous immunity against Schistosoma mansoni. bioRxiv [Preprint]. 2025 Feb 8:2025.02.06.636930. https://www.biorxiv.org/content/10.1101/2025.02.06.636930v1
- The Herbert Lab. https://drherbertlab.org/research.html
- The US Centers for Disease Control and Prevention. https://www.cdc.gov/parasites/about/index.html
- The US Centers for Disease Control and Prevention. https://www.cdc.gov/dpdx/schistosomiasis/index.html
- MSD Manual. https://www.msdmanuals.com/professional/infectious-diseases/trematodes-flukes/introduction-to-trematodes-flukes
- Written by Rebecca Kranz with Andrea Gwosdow, PhD at https://www.gwosdow.com

